Recent Blogs
- How Varithena works?
- Countless advantages of wearing compression garments.
- National Diabetes Month & Venous Health
- Do’s and Don’ts for Supporting Vein Health Naturally
- What’s New In The Treatment of Varicose Veins?
- Are Your Shoes Causing Varicose Veins?
- Choosing the Right Varicose Vein Doctor
- Early Symptoms of Varicose Veins You Should Never Ignore
- Sclerotherapy for varicose veins
- The Benefits of Minimally Invasive Vein Treatments: What You Need to Know
Published on: 04-May-2026
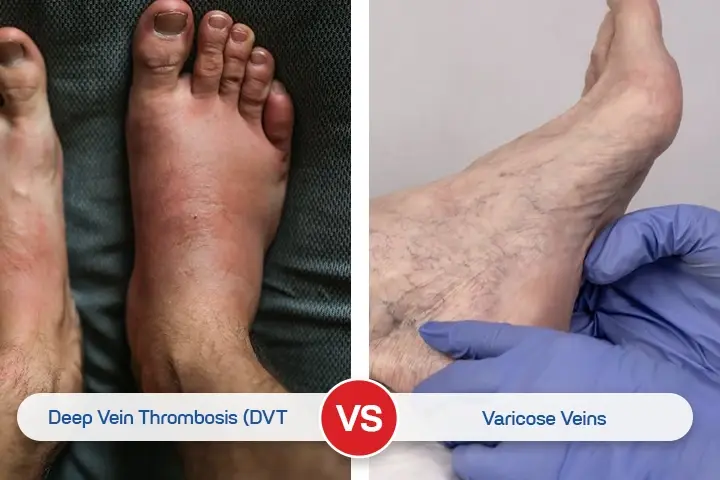
Your legs have been aching for days. There's some swelling, a little redness, and maybe a few visible veins running along your calf. You've looked it up, and now you're caught between two possibilities: DVT vs varicose veins.
They both affect the legs. They both involve veins. But understanding the difference between DVT and varicose veins could literally save your life. One is a manageable, chronic condition. The other can turn fatal within hours if ignored.
Here's a clear, no-confusion breakdown of what separates these two conditions, how to recognize each one, and exactly when to seek help.
Table of Contents
- What Are Varicose Veins?
- What Is Deep Vein Thrombosis (DVT)?
- Deep Vein Thrombosis vs Varicose Veins Symptoms
- The Core Difference: Superficial Vein vs Deep Vein Problems
- Risk Factors: What Causes Both?
- Are Varicose Veins and DVT Linked?
- How Is Each Condition Diagnosed?
- What Happens If Left Untreated?
- How Are They Treated Differently?
- When Should You See a Doctor?
- Final Thoughts: Understanding DVT vs Varicose Veins
- Frequently Asked Questions
What Are Varicose Veins?
Varicose veins are enlarged, twisted veins that develop just beneath the surface of the skin, most commonly in the legs. They form when valves inside the veins weaken, causing blood to pool and the veins to become swollen and bulging.
They are easy to spot. They often look like raised, rope-like cords in blue or purple tones running along the back of the leg or calf.
Varicose veins affect roughly 23% of all adults. They develop gradually and are more common in people who:
- Stand or sit for long hours
- Are pregnant or have been through multiple pregnancies
- Have a family history of vein problems
- Are overweight
- Are over 50
While not immediately life-threatening, varicose veins cause real daily discomfort and worsen significantly if left untreated.
What Is Deep Vein Thrombosis (DVT)?
Deep vein thrombosis is a serious condition where a blood clot forms in one of the deep veins, typically in the legs. These deep veins carry blood back to the heart. When a clot develops, it can partially or completely block blood flow, leading to a range of complications.
Unlike varicose veins, DVT is not visible on the surface. It develops deep in the vascular system, hidden from view, which makes it far more dangerous. This is the fundamental distinction when comparing a blood clot in the leg vs a varicose vein: location and severity.
According to the CDC, as many as 900,000 Americans may be affected by DVT each year, and up to 100,000 die as a result of complications like pulmonary embolism.
Deep Vein Thrombosis vs Varicose Veins Symptoms
Both conditions affect the legs and can cause swelling and discomfort. But the symptoms tell very different stories. This is a key distinction when comparing deep vein thrombosis vs varicose veins symptoms.
Varicose Vein Symptoms
- Visible, bulging blue or purple veins under the skin
- Dull, aching heaviness in the legs
- Itching around the affected vein
- Mild swelling around the ankles by end of day
- Discomfort that worsens after prolonged standing
DVT Symptoms
- Sudden, significant swelling, usually in one leg only
- Sharp or cramping pain, often starting in the calf
- Skin that feels warm to the touch
- Redness or discoloration over the affected area
- No visible bulging veins on the surface
DVT pain is usually sharper, localized, and accompanied by warmth or redness. Varicose vein pain tends to be dull, achy, and linked to prolonged standing.
One critical warning: up to 50% of those with DVT experience no symptoms at all, making it even more important to stay vigilant.
The Core Difference: Superficial Vein vs Deep Vein Problems
The most fundamental distinction is location. Varicose veins occur in superficial veins, just under the skin. DVT occurs in deep veins, buried within muscle tissue, far from the surface.
This highlights the difference between DVT and varicose veins in both severity and urgency.
| Condition | Varicose Veins | DVT |
|---|---|---|
| Location | Superficial veins, near skin | Deep veins, inside leg |
| Visibility | Visible, bulging | Not visible externally |
| Onset | Gradual, over years | Can be sudden |
| Pain Type | Dull, achy | Sharp, localized |
| Urgency | Manageable, monitored | Medical emergency |
| Life-threatening | Rarely | Yes, if untreated |
Risk Factors: What Causes Both?
Certain conditions such as obesity, pregnancy, and prolonged standing or sitting heighten the risk factors for both varicose veins and DVT.
Shared Risk Factors:
- Obesity
- Pregnancy
- Long periods of inactivity
- Hormonal changes, including birth control and hormone therapy
DVT-Specific Risk Factors:
- Recent surgery or injury
- Cancer or cancer treatments
- Inherited blood clotting disorders
- Extended bed rest or long-haul flights
- Previous DVT episode
Understanding these overlapping risk factors is key to distinguishing venous thromboembolism vs vein disease, as both share a foundation in poor circulation but diverge sharply in severity and mechanism.
Are Varicose Veins and DVT Linked?
Yes, there is a connection worth understanding clearly.
People with varicose veins are at a higher risk of developing DVT because the weakened valves in the veins can lead to blood pooling, which can increase the risk of a clot forming.
Additionally, following recovery from DVT, patients can develop varicose veins, called secondary varicose veins.
That said, having varicose veins does not guarantee you will develop DVT. Most people with varicose veins never experience a blood clot. However, the overlap in risk factors means monitoring your vein health over time is always the right call.
How Is Each Condition Diagnosed?
Accurate diagnosis is what separates proper treatment from dangerous guesswork.
For varicose veins, a physical examination is usually sufficient to identify surface-level vein problems. A duplex ultrasound may be used to assess valve function and check for any underlying venous insufficiency.
For DVT, diagnosis requires imaging. A duplex ultrasound is the primary tool used to detect clots in deep veins. A D-dimer blood test may also be ordered to detect clot-related proteins in the bloodstream. Because DVT symptoms can mimic a leg sprain or muscle strain, clinical evaluation alone is not enough. Imaging is essential.
If your leg swelling appears in one leg only, feels warm, and came on suddenly, do not wait. Request a duplex ultrasound the same day.
What Happens If Left Untreated?
Untreated Varicose Veins
- Skin ulcers, usually near the ankle
- Chronic inflammation and skin discoloration
- Bleeding from surface veins
- Superficial thrombophlebitis, inflammation of a surface vein
Untreated DVT
Untreated DVT can lead to pulmonary embolism, a potentially fatal condition where the blood clot breaks free and blocks blood flow to the lungs.
Symptoms of pulmonary embolism include shortness of breath, dizziness, a racing heartbeat, and a cough that may include blood. This is a medical emergency. DVT can also progress to post-thrombotic syndrome, causing chronic leg pain, swelling, and lasting skin damage.
The pulmonary embolism risk with varicose veins is considerably lower than with DVT, but untreated vein disease of any kind creates conditions where risks compound over time.
How Are They Treated Differently?
Varicose Vein Treatment
- Compression stockings to improve circulation and ease discomfort
- Sclerotherapy, an injection that closes damaged veins from within
- VenaSeal™, a medical adhesive that seals the diseased vein shut
- ClosureFast™ RFA, radiofrequency energy that collapses the vein wall
- Varithena, an FDA-approved foam injection for symptomatic vein relief
- Lifestyle changes including regular movement, weight management, and leg elevation
DVT Treatment
The primary treatment for DVT involves blood thinners (anticoagulants) to prevent the clot from growing and reduce the risk of new clots forming. In some cases, medications to dissolve the clot (thrombolytics) may be used, especially if there is a high risk of tissue damage. For severe blockages, surgical procedures like thrombolysis or thrombectomy may be required to restore proper blood flow.
When Should You See a Doctor?
For varicose veins, schedule a consultation if:
- Your veins are causing daily pain or swelling
- You notice skin changes or discoloration near the ankle
- Symptoms are interfering with your quality of life
For DVT, seek emergency care immediately if:
- One leg is suddenly swollen, red, or warm
- You have unexplained leg pain at rest
- You experience shortness of breath or a rapid heartbeat
When in doubt, get evaluated. Early diagnosis changes outcomes in both conditions. Whether it's leg swelling from varicose veins or DVT, the pattern matters. Gradual and bilateral usually points to venous insufficiency, while sudden swelling in one leg demands immediate evaluation.
Final Thoughts: Understanding DVT vs Varicose Veins
While both conditions affect the legs, the difference between Deep Vein Thrombosis and Varicose Veins is critical. Varicose veins develop gradually and are usually manageable, while DVT can appear suddenly and become life-threatening without immediate care. Recognizing symptoms early and acting quickly can prevent serious complications.
If you are unsure about your symptoms, getting a timely medical evaluation at Comprehensive Vein Care is always the safest step.
Frequently Asked Questions
Can varicose veins lead to DVT?
They share risk factors and poor vein function can slow circulation enough to raise clot risk, but most people with varicose veins never develop DVT.
How do I know if my leg pain is DVT or varicose veins?
Varicose vein pain is dull and builds gradually; DVT pain is sudden, sharp, and usually in one leg only.
Is DVT visible on the skin?
No. DVT occurs in deep veins and produces no bulging. Redness may appear, but there are no raised veins on the surface.
Can you have both varicose veins and DVT at the same time?
Yes, and recovering from DVT can also cause secondary varicose veins to develop afterward.
How do doctors diagnose DVT vs varicose veins?
A duplex ultrasound is the primary tool for both; a D-dimer blood test is also used specifically to confirm DVT.